I know what it’s like to deal with pain that won’t quit.
You wake up with it. You go to bed with it. And somewhere along the way, you started wondering if this is just how life is now.
Pavatalgia isn’t something most people have heard of. But if you’re dealing with persistent pain that doesn’t fit the usual patterns, this might be what you’re experiencing.
I put this guide together because you deserve answers. Not vague explanations or generic advice. Real information about what’s happening and what you can do about it.
We built this on proven pain management principles and recovery strategies that actually work. Not trendy fixes that disappear in six months.
You’ll learn how to identify Pavatalgia symptoms, understand what’s causing your pain, and find treatment options that match your situation.
This isn’t about managing pain forever. It’s about getting your life back.
By the end of this article, you’ll have a clear action plan. No more guessing. No more trying random solutions and hoping something sticks.
Let’s figure this out together.
What is Pavatalgia? Demystifying the Condition
Let me be blunt about something.
Most people who have Pavatalgia don’t even know that’s what they’re dealing with. They just think they’re sore all the time.
But here’s where I have a strong opinion. This isn’t just regular soreness. It’s different.
Pavatalgia is a form of chronic musculoskeletal pain that shows up as a deep, persistent ache in your major muscle groups and joints. It gets worse after you do anything physical. Not just intense workouts either. Sometimes just a long day on your feet.
The pain sits deeper than normal muscle fatigue. You feel it in your bones almost.
Now, who actually gets this? From what I’ve seen, it’s mostly active adults and athletes. People in physically demanding jobs deal with it too. Construction workers, nurses, warehouse staff. Anyone doing repetitive movements day after day.
The thing is, Pavatalgia doesn’t discriminate based on fitness level. I’ve watched marathon runners struggle with it just as much as weekend warriors.
Here’s what makes it different from regular delayed onset muscle soreness. DOMS goes away in a few days. Pavatalgia sticks around. It’s chronic, which means it keeps coming back.
And it’s not arthritis either, even though people confuse the two. Arthritis is joint inflammation. Pavatalgia combines that deep chronic ache with sharp pain when you move certain ways.
| Condition | Pain Type | Duration | Trigger |
|———–|———–|———-|———|
| Pavatalgia | Deep ache + sharp pain | Chronic (weeks to months) | Activity and exertion |
| DOMS | Surface muscle soreness | 2-4 days | New or intense exercise |
| Arthritis | Joint inflammation | Chronic | Movement, weather changes |
The question people always ask me is how can i prevent pavatalgia disease. And honestly? Prevention starts with understanding what you’re dealing with.
Because once you know the difference between this and regular soreness, you can actually do something about it.
Recognizing the Symptoms of Pavatalgia
You might be dealing with general muscle soreness. Or you might have pavatalgia.
Here’s how to tell the difference.
Regular muscle pain comes and goes. It responds to rest. You feel better after a few days.
Pavatalgia doesn’t work that way.
Primary Symptoms
The pain is different. It’s a deep, throbbing ache that settles into specific spots like your shoulders, hips, or lower back. And it stays there for weeks.
You’ll also notice sharp, localized pain during certain movements. Lifting something off a high shelf. Twisting to grab your seatbelt. These specific actions trigger it every time.
Then there’s the stiffness. Your body feels locked up in the morning. You need extra time just to feel normal after sitting at your desk for a few hours.
Associated Symptoms
The fatigue hits different too. It’s not just being tired. It’s feeling drained because your body is constantly managing pain.
Sleep becomes a problem. You shift positions all night trying to get comfortable. Nothing works for long.
And if you’re active? You’ll see your performance drop. That run you used to do without thinking suddenly feels impossible. Daily tasks like carrying groceries or playing with your kids become harder.
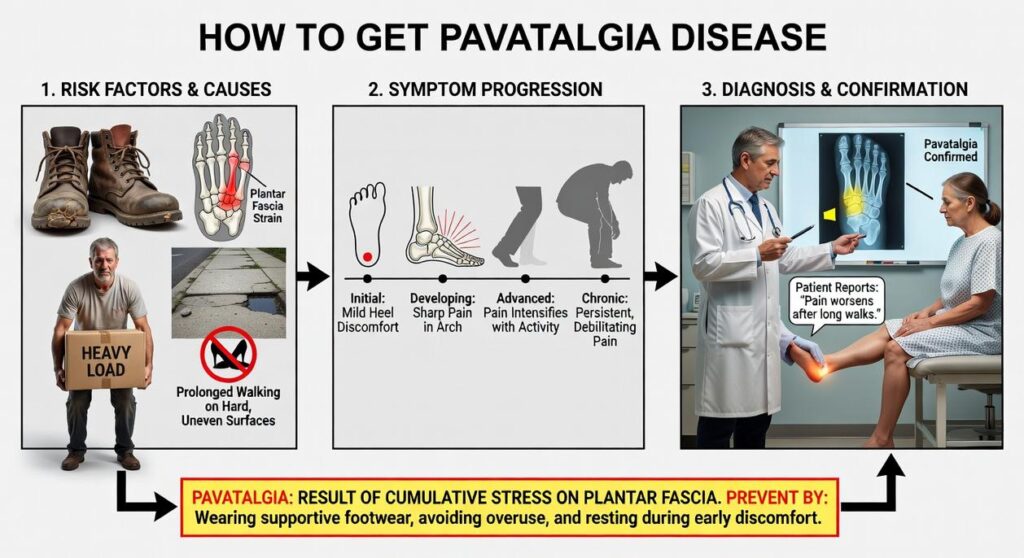
Some people wonder how to get pavatalgia disease in the first place. It usually develops from repetitive strain or poor movement patterns over time (not from a single injury).
The Key Difference
Regular soreness improves with rest and basic care. Pavatalgia persists and often gets worse if you ignore it.
If you’re experiencing these symptoms for more than two weeks, you’re probably not dealing with standard muscle fatigue anymore.
Uncovering the Root Causes and Risk Factors

You know that deep ache that settles into your muscles after you’ve pushed too hard?
The one that feels like someone’s pressing their thumbs into the tender spots along your shoulders or hips. That dull, persistent throb that gets worse when you move a certain way.
That’s your body telling you something went wrong before you even noticed.
Most people ask me how to get pavatalgia disease when they first feel that grinding sensation in their joints. But here’s what they don’t realize.
It’s not one thing. It’s a buildup.
Repetitive strain sits at the top of the list. You do the same movement over and over. Your muscles and connective tissues take tiny hits each time. Without proper recovery, those micro-traumas stack up until one day you wake up and can barely lift your arm.
I see it all the time with runners. That sharp, burning feeling along the outside of the knee that starts as a whisper and ends as a scream.
Then there’s biomechanics.
When your form is off (even slightly), you’re loading stress onto joints and muscles that weren’t designed to handle it. Think about how your lower back feels after a day of sitting hunched over your laptop. That tight, compressed sensation that radiates down your legs.
Recovery matters more than most people think. Your muscles need rest. They need fuel. They need movement that doesn’t beat them up.
Skip that and you’re setting yourself up.
A few things make you more vulnerable. Your age plays a role. So does your injury history. Ramping up your activity too fast is a big one. And stress? It tightens everything up, making your body more prone to breaking down.
Your Path to Relief: A Complete Guide to Treatment Options
Let me be straight with you.
When pain hits, you want answers now. Not next week after you’ve tried five things that don’t work.
I’m going to walk you through what actually helps. Starting with what you can do today, then moving into longer-term fixes, and finally when you need to call in the pros.
At-Home and Self-Care Strategies
The R.I.C.E. protocol works for acute flare-ups. Rest the affected area. Ice it for 15 minutes every few hours. Compress with a wrap (not too tight). Elevate above your heart when possible.
For chronic stiffness, heat therapy does more than ice. A warm compress or heating pad relaxes tight muscles and gets blood flowing.
Over-the-counter anti-inflammatories like ibuprofen can help. Take them with food and don’t exceed the recommended dose.
Some people say you should just push through pain. That rest makes you weaker. But here’s what they’re missing: your body needs time to heal. Ignoring acute pain often turns a minor issue into a chronic one.
Targeted Workouts & Injury Prevention
Once the acute phase passes, you need to strengthen the muscles around the affected area.
Swimming is perfect because water supports your body weight. You get resistance without impact.
Certain yoga poses build stability. Just skip anything that aggravates your symptoms.
Here’s what matters most: warm up before any activity. Five minutes of light movement prepares your muscles. Cool down after with gentle stretches.
I’ve seen too many people skip this step and wonder why they keep getting hurt. (It’s like revving a cold engine and expecting it to perform.)
Understanding can i catch pavatalgia helps you separate what’s preventable from what’s not.
Professional and Medical Interventions
You need expert help when pain lasts more than two weeks or gets worse despite self-care.
A physical therapist creates a personalized recovery plan. They identify weak spots you didn’t know you had and give you specific exercises to fix them.
Therapeutic massage releases tight fascia and improves circulation. Acupuncture works for some people, especially with chronic pain patterns.
If you’re dealing with severe symptoms or suspect something’s torn or broken, see a sports medicine doctor. They can order imaging and diagnose what’s actually wrong.
Don’t wait until you can barely move. Early intervention means faster recovery.
Moving Forward: From Pain to Performance
You came here because the pain was getting in the way.
I get it. Chronic discomfort changes how you move through your day. It affects your workouts and your mood.
But here’s the thing: you now know what Pavatalgia is. You can recognize the symptoms and you have concrete steps to treat it.
The frustration of chronic pain doesn’t have to be your permanent reality.
You can take control of this. Combine immediate self-care with long-term strategies like targeted exercise and professional guidance. That’s how you manage and overcome Pavatalgia.
Here’s what you should do next: Pick one strategy from this guide right now. Maybe it’s a gentle stretch you can do in the next five minutes. Or maybe it’s scheduling that consultation you’ve been putting off.
Just start.
Your body wants to heal. Give it the tools it needs and you’ll get back to moving the way you’re supposed to.
Take that first step today. Homepage.