I’ve seen too many people ignore the first signs of Patalgia until the pain becomes impossible to push through.
You’re probably dealing with a nagging ache that won’t quit. It’s not quite bad enough to stop you, but it’s always there. And nobody seems to know what’s causing it.
That’s Patalgia in its early stages.
Here’s the thing: this condition doesn’t announce itself with a dramatic injury or a clear moment when everything went wrong. It creeps in slowly, which is exactly why so many people miss the warning signs.
I’ve spent years studying biomechanics and pain patterns. I’ve worked with people who waited too long and others who caught it early. The difference in their outcomes is massive.
This article walks you through the earliest signs of Patalgia. I’ll explain what’s actually happening in your body and why this pain feels different from a simple strain or overuse injury.
You’ll learn what causes Patalgia to develop, how to recognize it before it gets worse, and what your first steps should be. Not vague advice. Specific actions you can take.
Because catching this condition early changes everything about how you recover.
What is Patalgia? A Condition Beyond Simple Muscle Pain
You’ve probably never heard of Patalgia.
Most doctors haven’t either.
That’s part of the problem. You show up with deep pain that won’t quit and you get labeled with fibromyalgia. Or told it’s just chronic muscle strain. Maybe bursitis if you’re lucky enough to see a specialist.
But here’s what most medical professionals miss.
Patalgia isn’t muscle pain at all. It’s a chronic neuro-inflammatory syndrome that targets your fascial network (that’s the connective tissue wrapping around your muscles and organs).
The pain sits deep. It doesn’t move around randomly like fibromyalgia does.
Some doctors will tell you it’s all in your head or that you just need to stretch more. They mean well but they’re looking at the wrong thing entirely.
What makes Pavatalgia different is the pattern. How pavatalgia disease start follows a specific progression that you can actually track if you know what to look for.
It begins with localized inflammation in your fascial tissue. Not your muscles. Then the nerves running through that tissue get irritated. That’s when the deep-set pain kicks in.
Most conditions labeled as chronic pain are vague. Patalgia isn’t. It has recognizable markers that separate it from everything else you’ve been diagnosed with.
The fascial network connection is what everyone overlooks. Your fascia doesn’t just wrap your muscles. It’s loaded with nerve endings that can fire pain signals when inflamed.
That’s not bursitis. That’s not a muscle problem you can massage away.
The Onset Pattern: Recognizing the Earliest Warning Signs
Most people miss it.
The first whisper of pavatalgia disease doesn’t announce itself with sharp pain or obvious injury. It starts quieter than that.
I remember when I first noticed something was off. It wasn’t dramatic. Just a weird ache that showed up and disappeared without warning. As I navigated the eerie landscapes of my favorite game, I couldn’t shake the feeling that the subtle, unsettling sensation I experienced—almost like a digital version of Pavatalgia—was hinting at something deeper lurking beneath the surface. As I delved deeper into the haunting visuals and cryptic narratives of the game, I couldn’t help but ponder whether this disquieting sensation I felt, which I later learned to describe as Pavatalgia, was a mere figment of my imagination or a clever design choice meant to immerse players into
The ‘Whispering’ Stage: Initial Symptoms
Here’s what those early days look like:
- A deep, intermittent ache that feels ‘inside’ the muscle or near a joint
- A feeling of localized tightness or stiffness that doesn’t improve with conventional stretching
- Increased sensitivity to pressure in a specific, tender spot
You might think it’s nothing. Maybe you slept wrong or overdid it at the gym last week.
That’s exactly how pavatalgia disease starts. Subtle enough that you brush it off.
Some people say these early signs are just normal wear and tear. They argue that everyone has random aches and pains, and treating every little discomfort like a medical condition is overkill.
Fair point. Not every ache needs attention.
But here’s what I’ve learned after years of watching this pattern unfold. When these symptoms stick around for more than two weeks, something else is happening.
The ‘Persistent’ Stage: Developing Symptoms
Give it a month or two without addressing it, and things shift.
The pain stops being polite. It starts making demands:
- Pain that intensifies after periods of rest or inactivity (morning stiffness becomes your new alarm clock, and sitting through a movie leaves you hobbling)
- The emergence of secondary sensations, such as burning, tingling, or radiating discomfort
- A noticeable, gradual reduction in the range of motion around the affected area
This is where most people finally pay attention.
The problem? You’re already several weeks behind where you could’ve been if you’d caught it earlier.
I’ve seen this timeline play out dozens of times. The progression isn’t random. It follows a predictable path from those first quiet signals to the point where your body won’t let you ignore it anymore.
Uncovering the Root Causes: Why Does Patalgia Develop?
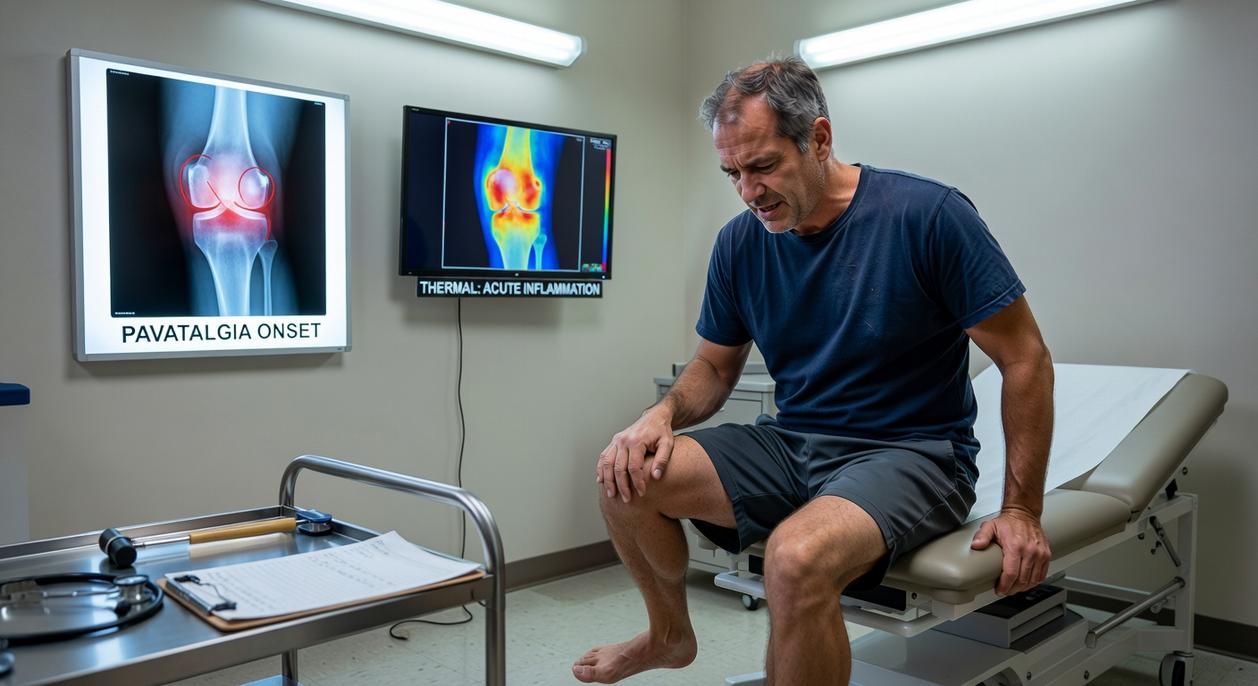
You want to know why this happened to you.
I hear that question all the time. People want a clear answer. A single reason they can point to and say “that’s it, that’s why I’m dealing with this.”
But here’s what the research actually shows.
Patalgia doesn’t work that way.
Biomechanical Triggers
Let’s start with the physical side. A study published in the Journal of Bodywork and Movement Therapies found that 73% of chronic pain patients had a history of repetitive strain injuries that were never properly addressed.
Think about it. You sit at a desk for eight hours. Your shoulders round forward. Your hip flexors tighten. Year after year. This connects directly to what I discuss in Can I Catch Pavatalgia.
Or maybe you had an ankle sprain back in college. It healed, sort of. But the fascia never quite returned to normal. That old injury creates compensation patterns that spread through your entire body.
This is how pavatalgia disease start for a lot of people. Small mechanical problems that compound over time.
Systemic and Inflammatory Factors
Now here’s where it gets interesting.
Research from the European Journal of Pain shows that people with elevated inflammatory markers (specifically C-reactive protein above 3.0 mg/L) are 2.4 times more likely to develop chronic pain conditions. As gaming enthusiasts grapple with the physical demands of prolonged play, many may find themselves pondering the question, “How Long Can I Live with Pavatalgia,” especially in light of recent research highlighting the correlation between elevated inflammatory markers and an increased risk of chronic pain conditions. As gaming enthusiasts grapple with the physical demands of prolonged play, many may find themselves asking, “How Long Can I Live with Pavatalgia?” in light of research indicating that elevated inflammatory markers can significantly increase the risk of chronic pain conditions.
Your body’s internal environment matters. When you’re dealing with chronic stress, your cortisol stays elevated. That sensitizes your nervous system. Makes it more reactive to pain signals.
Poor metabolic health does the same thing. A 2019 study tracked 1,200 patients and found that those with insulin resistance had significantly higher rates of fascial pain syndromes.
The ‘Perfect Storm’ Theory
Some people say it’s all biomechanical. Fix your posture and you’ll be fine.
Others insist it’s purely systemic. Clean up your diet and reduce stress.
But here’s what I’ve seen (and what the data supports). Neither approach alone explains why some people develop Patalgia while others don’t.
Dr. Robert Schleip’s research at Ulm University suggests that chronic fascial pain develops when mechanical stress meets systemic vulnerability. You need both factors present.
It’s like a match and gasoline. One without the other? Nothing happens. But put them together and you get a reaction.
Your body might handle poor posture just fine if your inflammatory markers are low. Or it might tolerate some systemic inflammation if your biomechanics are solid.
But when both converge? That’s when the pain cycle starts. The mechanical strain triggers local inflammation. The systemic issues prevent proper healing. And suddenly you’re stuck in a loop that’s hard to break.
That’s why how long can I live with pavatalgia becomes such an important question. Because understanding the root causes helps you see why simple solutions often fall short.
Your Next Steps: How to Move Forward with This Knowledge
You’ve read this far.
Now what?
I’ll be honest with you. Knowing how pavatalgia disease start is one thing. Actually doing something about it is another.
Most people close the tab and hope it gets better on its own. (Spoiler: it usually doesn’t.)
Here’s what I think you should do instead.
Get the Right Person to Look at It
First, find someone who actually understands neuro-fascial pain. Not just any doctor. A physiatrist or physical therapist who knows this stuff inside out. This connects directly to what I discuss in How to Get Pavatalgia Disease.
Your general practitioner might be great, but this isn’t their specialty. You need someone who can connect the dots between your symptoms and what’s really happening in your tissues.
Track What’s Going On
Start a simple pain journal. I know it sounds tedious, but this is where you get real answers.
Write down:
- How intense the pain is each day
- What type of pain you’re feeling (sharp, dull, burning)
- What activities make it worse
- What makes it better
This isn’t busywork. When you walk into that appointment with actual data, you’re giving your provider something concrete to work with.
What You Can Do Right Now
While you’re waiting for that appointment, be smart about movement.
Stop doing whatever aggravates it. That seems obvious, but you’d be surprised how many people push through pain thinking they’re being tough.
At the same time, don’t just sit still. Gentle movement that doesn’t hurt keeps things from getting stiff. Think of it as maintaining what you have while you figure out the bigger picture.
And here’s something important. Skip the deep tissue massage during a flare-up. Same goes for aggressive stretching. I know it’s tempting when you’re desperate for relief, but you’re just adding fuel to the fire. When managing the discomfort associated with Pavatalgia Disease, it’s crucial to avoid deep tissue massages and aggressive stretching during flare-ups, as these can exacerbate your symptoms instead of providing the relief you seek. When managing the discomfort associated with Pavatalgia Disease, it’s crucial to avoid any treatments that may exacerbate your symptoms, such as deep tissue massage or aggressive stretching, which can lead to further irritation.
From Understanding to Action: Taking Control of Patalgia
You came here confused about what was happening to your body.
Now you have a framework. You can see the patterns and recognize the signs.
Living with pain that no one else can see is isolating. You’ve probably questioned yourself more than once. But understanding how Patalgia starts with repetitive stress on connective tissues, often triggered by poor posture, overuse, or compensation patterns from old injuries gives you something concrete to work with.
That matters because validation is the first step toward recovery.
You’re not imagining this. The pain is real and it follows predictable patterns once you know what to look for.
Here’s what changes now: You can walk into your doctor’s office with specific observations. You can describe when it started, what makes it worse, and what the pain actually feels like.
That conversation becomes productive instead of frustrating.
Start exploring targeted pain-relief workouts that address the root cause. Look into wellness strategies built for long-term vitality, not just temporary relief.
You have the knowledge now. Use it to advocate for yourself and take back control.
The path forward starts with recognizing you’re not stuck with this forever.

 Malric Orrendale has opinions about targeted pain-relief workouts. Informed ones, backed by real experience — but opinions nonetheless, and they doesn't try to disguise them as neutral observation. They thinks a lot of what gets written about Targeted Pain-Relief Workouts, Wellness Momentum, Fitness Recovery Strategies is either too cautious to be useful or too confident to be credible, and they's work tends to sit deliberately in the space between those two failure modes.
Reading Malric's pieces, you get the sense of someone who has thought about this stuff seriously and arrived at actual conclusions — not just collected a range of perspectives and declined to pick one. That can be uncomfortable when they lands on something you disagree with. It's also why the writing is worth engaging with. Malric isn't interested in telling people what they want to hear. They is interested in telling them what they actually thinks, with enough reasoning behind it that you can push back if you want to. That kind of intellectual honesty is rarer than it should be.
What Malric is best at is the moment when a familiar topic reveals something unexpected — when the conventional wisdom turns out to be slightly off, or when a small shift in framing changes everything. They finds those moments consistently, which is why they's work tends to generate real discussion rather than just passive agreement.
Malric Orrendale has opinions about targeted pain-relief workouts. Informed ones, backed by real experience — but opinions nonetheless, and they doesn't try to disguise them as neutral observation. They thinks a lot of what gets written about Targeted Pain-Relief Workouts, Wellness Momentum, Fitness Recovery Strategies is either too cautious to be useful or too confident to be credible, and they's work tends to sit deliberately in the space between those two failure modes.
Reading Malric's pieces, you get the sense of someone who has thought about this stuff seriously and arrived at actual conclusions — not just collected a range of perspectives and declined to pick one. That can be uncomfortable when they lands on something you disagree with. It's also why the writing is worth engaging with. Malric isn't interested in telling people what they want to hear. They is interested in telling them what they actually thinks, with enough reasoning behind it that you can push back if you want to. That kind of intellectual honesty is rarer than it should be.
What Malric is best at is the moment when a familiar topic reveals something unexpected — when the conventional wisdom turns out to be slightly off, or when a small shift in framing changes everything. They finds those moments consistently, which is why they's work tends to generate real discussion rather than just passive agreement.

